THE PROGRESSIVE DECLINE OF HYALURONIC ACID AND HOW IT SHAPES THE SKIN
Laura Masini, JetPeel by TavTech Global Educator
ABSTRACT
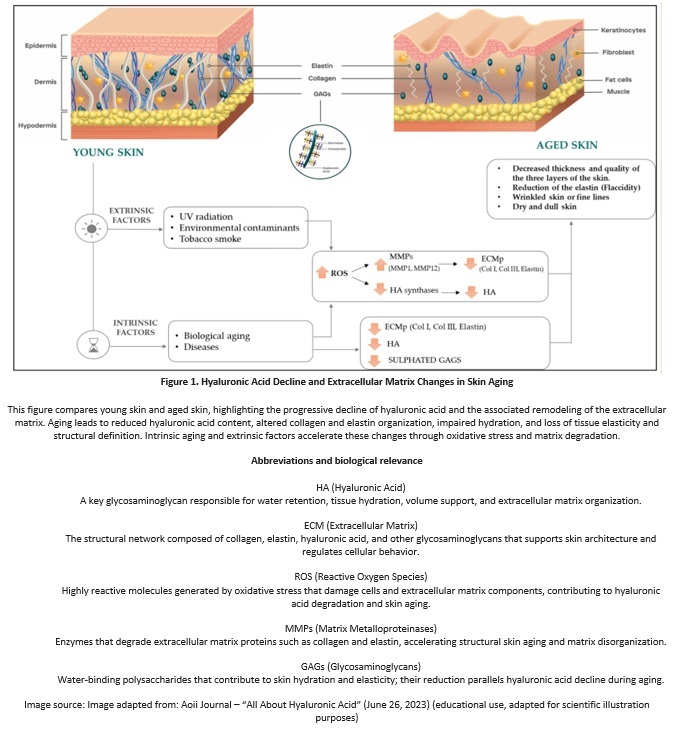
Hyaluronic acid (HA) is one of the most relevant biological molecules shaping skin quality and facial architecture. Naturally present within the skin, it belongs to the family of glycosaminoglycans, sugar-based molecules characterized by a remarkable capacity to bind and retain water. Its unique capacity to bind and retain water makes it a key regulator of skin hydration, volume, and mechanical resistance.
Beyond hydration, hyaluronic acid plays a structural role by maintaining tissue spacing, flexibility, and resilience. It allows the skin to absorb mechanical stress, preserve elasticity, and maintain a stable yet adaptable architecture. As hyaluronic acid progressively declines with age, its loss triggers a cascade of changes affecting hydration, structural integrity, and tissue behavior. The skin gradually loses its ability to maintain volume and resistance, leading to visible alterations in texture, tone, and facial shape.
INTRODUCTION
Hyaluronic acid is a fundamental component of skin homeostasis, regulating hydration, extracellular matrix organization, and tissue biomechanics. Its progressive decline constitutes an early biological event that precedes overt skin aging and contributes to cumulative structural and functional alterations. Reduced hyaluronic acid availability compromises internal tissue organization, mechanical stability, and adaptive capacity, thereby influencing the skin’s response to mechanical and environmental stressors.
HYALURONIC ACID
Hyaluronic acid is a naturally occurring glycosaminoglycan produced by the skin as part of its normal physiological function. As a structural macromolecule, it plays a central role in water binding and regulation of tissue hydration. In the skin, hyaluronic acid is synthesized predominantly by dermal fibroblasts and released into the extracellular matrix, where it contributes to tissue volume, elasticity, and resistance to mechanical stress.
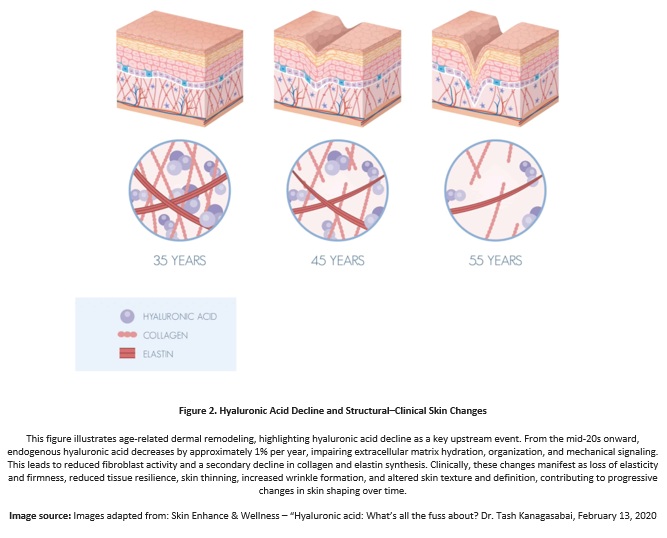
Smaller, functionally distinct amounts are synthesized by epidermal keratinocytes and endothelial cells, supporting surface hydration, epidermal turnover, barrier integrity, and local vascular dynamics. From approximately the mid-20s onward, hyaluronic acid progressively declines at an estimated rate of about 1% per year, affecting both its quantity and functional quality.
This decline accelerates with age as a result of reduced synthesis, increased enzymatic degradation, chronic inflammation, oxidative stress, and progressive extracellular matrix disorganization. Consequently, tissue hydration becomes uneven, mechanical responsiveness diminishes, and the skin gradually loses compactness, resilience, and structural definition, directly impacting skin quality and shaping.
WHY HYALURONIC ACID DECLINES AND WHAT ACCELERATES THE PROCESS
Hyaluronic acid decline reflects a progressive loss of skin homeostasis rather than an isolated effect of aging. Age-related changes in the dermal microenvironment weaken the biochemical and mechanical signals that regulate cellular activity.
As mechanotransduction (the cellular mechanism by which mechanical forces are sensed and converted into biological signals) becomes less efficient, fibroblast function progressively declines, leading to reduced synthesis and impaired organization of hyaluronic acid, collagen, and elastin. Cellular senescence further limits regenerative capacity. Although this process is physiologic, it is accelerated by external factors such as chronic ultraviolet exposure, pollution, smoking, and prolonged stress, which increase oxidative stress and inflammation.
HYALURONIC ACID DECLINE AND STRUCTURAL SKIN SHAPING
Hyaluronic acid plays a central role in maintaining skin structure by regulating hydration, mechanical stability, and cellular communication. Its decline is not merely a secondary consequence of aging, but represents an early structural alteration that progressively modifies how the skin functions and organizes itself over time. Hyaluronic acid homeostasis depends on a balance between synthesis by fibroblasts and enzymatic degradation by hyaluronidases.
With aging, inflammation, oxidative stress, and environmental exposure, synthesis gradually decreases while degradation accelerates. As this balance is disrupted, hyaluronic acid becomes increasingly fragmented and unevenly distributed within the extracellular matrix. The resulting loss of organized water retention compromises internal support and tissue repair efficiency. Fibroblasts, which rely on a hyaluronic-acid–rich microenvironment to maintain optimal activity, progressively reduce their function. This contributes to decreased collagen and elastin fiber production, leading to reduced tensile strength and elastic recoil.
Consequently, the skin gradually loses adaptability, resilience, and structural definition, altering skin and facial shaping over time. Preserving hyaluronic acid balance and matrix coherence is therefore essential to maintain skin structure before
internal disorganization becomes established and difficult to reverse
MANAGING HYALURONIC ACID DECLINE IN AESTHETIC MEDICINE
Addressing the progressive decline of hyaluronic acid requires an integrative, biologically oriented strategy rather than a purely corrective or volumetric approach. The reduction of endogenous hyaluronic acid results not only in impaired hydration, but also in extracellular matrix disorganization, diminished fibroblast activity, and secondary reductions in collagen and elastin synthesis.
These changes manifest as decreased skin density, elasticity, and firmness, contributing to skin thinning, increased fragility, reduced mechanical resistance, and diminished adaptive capacity. Effective intervention should combine hyaluronic acid replenishment with strategies that support dermal structure by supporting collagen and elastin function, rather than relying on hydration alone.
The use of JetPeel by TavTech, a non-invasive, needle-free, and no-contact technology, aligns with this approach by respecting the increased tissue fragility and reduced adaptive capacity associated with hyaluronic acid decline, while avoiding additional mechanical or inflammatory stress. It is supported by the use of JetCare Med by TavTech infusion formulations, including, osmolytes-enriched solutions, which act as effective carriers to protect peptides and improve protein stability.
These contribute to healthier, energized, and invigorated collagen and elastin, clinically proven to improve skin density, firmness, and elasticity. Rather than being framed as a corrective or aggressive intervention, this combined approach is compatible with current understanding of aging skin physiology, as it remains within known biological constraints related to hydration balance, matrix organization, cellular stability and skin aging physiology.
CONCLUSION
The progressive decline of hyaluronic acid represents a central biological event in skin aging, leading to extracellular matrix disorganization, reduced fibroblast activity, and progressive impairment of collagen and elastic fiber integrity.
These alterations compromise skin homeostasis, progressively affecting skin function and structural stability with evident reductions in density, firmness, elasticity, and adaptive capacity. Effective strategies must be aligned with the altered physiology of aging tissue and aimed at restoring skin structure and function rather than providing isolated corrective effects.
JetPeel by TavTech, together with JetCare Med infusion formulations, operate within physiological constraints while avoiding additional mechanical or inflammatory stress. This strategy contributes to improved skin density, firmness, and elasticity, effectively counteracting the structural consequences of hyaluronic acid decline and supporting functional skin remodeling over time.