MECHANISM OF CUTANEOUS PIGMENTATION AND TONE IRREGULARITIES
Laura Masini, JetPeel by TavTech Global Educator
ABSTRACT
Cutaneous pigmentation is a regulated biological process essential for skin color and photoprotection. This balance depends on coordinated melanocyte activity, melanin distribution, and epidermal turnover. Aging, inflammation, oxidative stress, and environmental exposure can disrupt this system, leading to pigment imbalance and tone irregularities.
Hyperpigmentation therefore reflects a loss of cutaneous homeostasis, characterized by melanocyte hyper-responsiveness, altered melanin distribution, and delayed epidermal clearance.
INTRODUCTION
Skin pigmentation represents the visible expression of a complex biological balance involving epidermal, dermal, and vascular components. Melanocyte activity, melanin transfer, keratinocyte turnover, and barrier function operate as an integrated system to ensure photoprotection and tone uniformity.
When disrupted by inflammatory stimuli, oxidative stress, hormonal influences, environmental aggression, or age-related changes, pigment regulation becomes altered. Slowed epidermal renewal and impaired dermal–epidermal communication favor melanin retention, increasing the persistence and visibility of pigmentation and leading to tone irregularities.
MELANIN IN THE SKIN
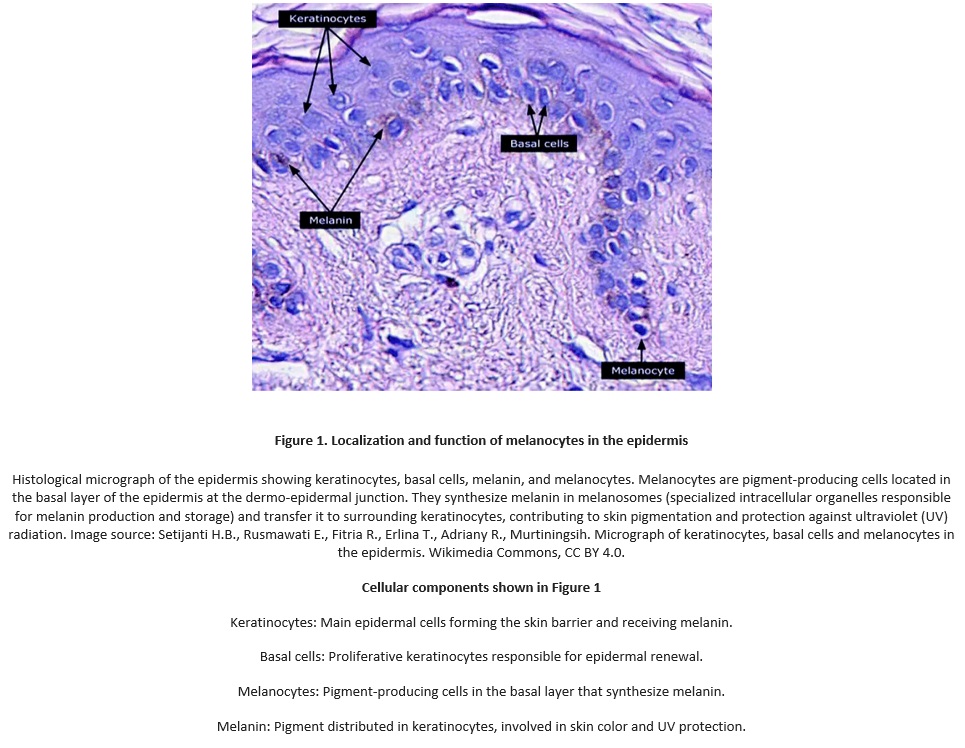
Melanin is a multifunctional biological pigment whose primary cutaneous role is photoprotection and the maintenance of skin homeostasis. It is produced by melanocytes located in the basal layer of the epidermis at the dermo-epidermal junction.
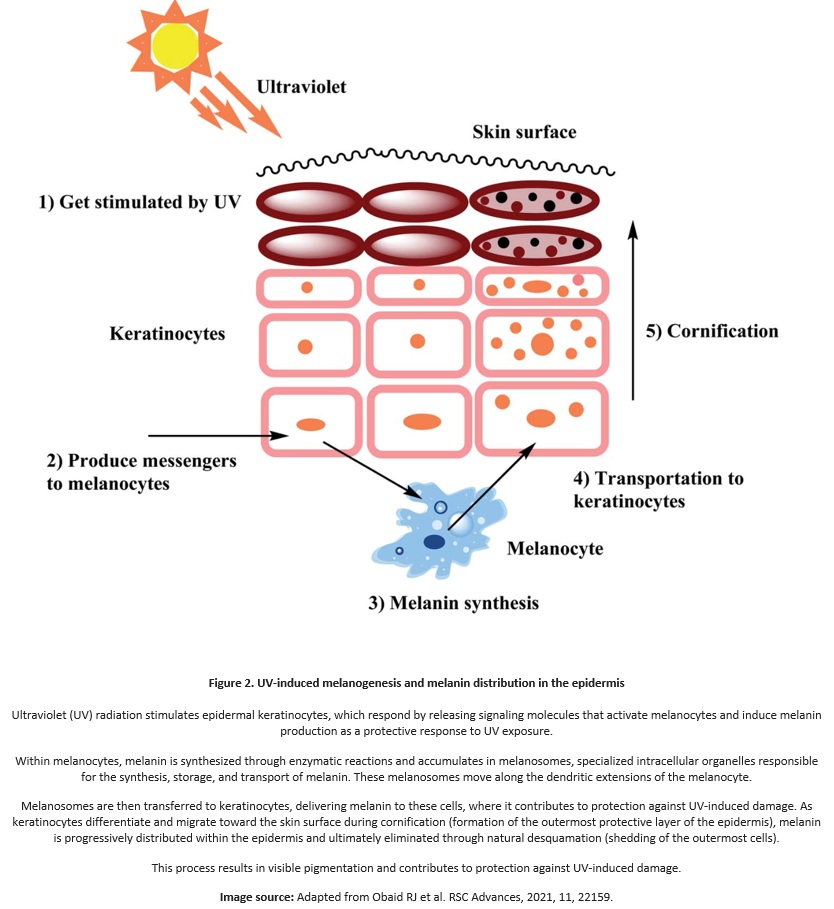
Each melanocyte interacts with approximately 30–40 keratinocytes, forming the epidermal melanin unit, which allows efficient protection of a large population of epidermal cells. Melanin production is primarily stimulated by solar radiation, particularly ultraviolet B (UVB), while ultraviolet A (UVA) contributes indirectly through oxidative stress.
High-energy visible light, inflammation, oxidative stress, hormonal signals, and mechanical or chemical irritation may also activate melanogenesis. Melanin synthesis occurs through melanogenesis, a tyrosinase-regulated biochemical process. Melanin is transferred to keratinocytes and positioned above the nucleus, forming a supranuclear cap that protects DNA and reduces oxidative stress. Epidermal melanin is eliminated through keratinocyte migration and desquamation, a process that slows with aging
PIGMENTATION ALTERATION AND LOSS OF CUTANEOUS BALANCE
Pigmentation alterations occur when cutaneous homeostasis is disrupted and the skin loses its ability to regulate melanocyte activity, melanin distribution, and pigment elimination in a coordinated manner. Under physiological conditions, melanin production is controlled, evenly distributed, and temporary. When this balance is altered, multiple aggravating factors promote the development and persistence of hyperpigmentation.
Aging plays a central role by slowing epidermal turnover, reducing cellular renewal, and decreasing the efficiency of melanin clearance, allowing pigment to remain within the skin for longer periods. Structural changes in the dermis, including reduced collagen and elastin support, impair communication between fibroblasts, keratinocytes, and melanocytes. Fibroblasts normally regulate melanocyte activity by providing structural support and releasing modulatory signals that limit excessive melanogenesis.
When dermal structure is altered, this regulatory control becomes less effective, indirectly favoring increased melanogenic stimulation. Barrier dysfunction further amplifies this process by increasing trans-epidermal water loss and maintaining chronic low-grade inflammation. In addition, melanocyte activity may be stimulated by chemical triggers, such as irritative or inflammatory agents, which can activate pigment production even in the absence of ultraviolet exposure. Vascular alterations contribute by sustaining the delivery of inflammatory mediators and reactive oxygen species, prolonging melanocyte stimulation over time.
At the epidermal level, altered melanin transfer and uneven spatial distribution lead to focal pigment accumulation within basal keratinocytes and the immediately adjacent lower suprabasal layers of the epidermis. In these layers, melanin is produced and initially distributed; when keratinocyte migration is delayed, pigment is retained instead of being progressively eliminated through desquamation. As a result, melanin persists and gradually becomes clinically visible as stable or recurrent hyperpigmentation. Therefore, pigmentation alterations reflect the combined effect of impaired homeostasis, altered dermal support, chemical and inflammatory stimulation, uneven pigment distribution, and delayed clearance, rather than melanin overproduction alone.
COMMON CLINICAL FORMS OF HYPERPIGMENTATION
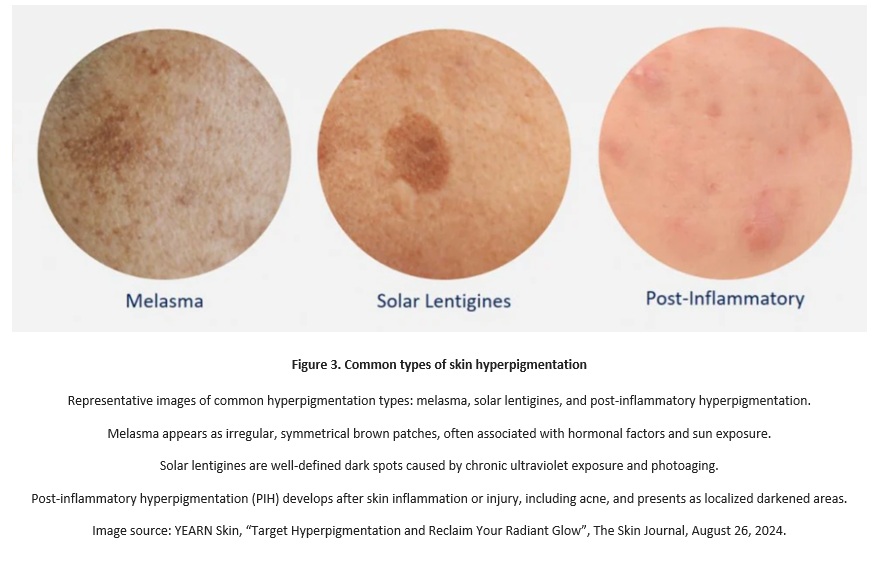
Hyperpigmentation may present in different clinical forms, depending on the underlying triggers, depth of pigment deposition, and biological behavior of melanocytes. Sun-induced hyperpigmentation, commonly referred to as sunspots or age spots (solar lentigines), typically develops in chronically photo exposed areas and results from cumulative ultraviolet damage, local melanocyte overactivity, and age-related reduction in pigment clearance.
These lesions are usually well-defined and reflect long-term imbalance between melanin production and elimination. Post-inflammatory hyperpigmentation arises following cutaneous inflammation or injury, such as acne, procedures, or irritation, and is driven by inflammatory mediators that stimulate melanocytes and alter pigment distribution during skin repair.
Melasma represents a more complex form of hyperpigmentation, primarily associated with hormonal influences, but strongly modulated by ultraviolet exposure, visible light, genetic predisposition, and vascular and inflammatory components. It is characterized by a diffuse, often symmetrical pattern and a tendency toward recurrence due to persistent melanocyte hypersensitivity. Although these conditions differ in origin and presentation, they share a common pathophysiological background of disrupted cutaneous homeostasis, making accurate identification of triggers and mechanisms essential for effective aesthetic management.
NON-INVASIVE AESTHETIC MANAGEMENT OF HYPERPIGMENTATION
The management of hyperpigmentation should be primarily based on non-invasive modalities, particularly in conditions characterized by inflammation, melanocyte hypersensitivity, and altered cutaneous homeostasis. Aggressive or invasive treatments may further destabilize the skin and increase the risk of chronic or post-inflammatory hyperpigmentation. Non-invasive approaches allow a gradual and controlled improvement of pigmentary alterations while preserving skin physiology. Gentle stimulation of the skin supports microcirculation and promotes controlled exfoliation, facilitating epidermal renewal and improved cell turnover.
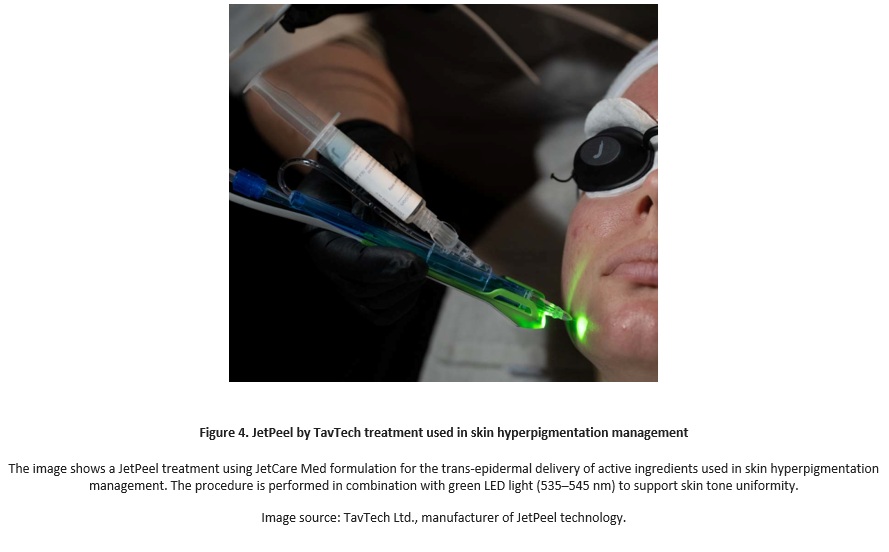
These mechanisms contribute to a more efficient and physiological elimination of excess melanin while minimizing inflammatory stress. Jet Peel by TavTech represents a non-invasive modality suitable for the management of hyperpigmented skin. Its mechanism of action enables effective skin stimulation without mechanical trauma, supporting circulation, oxygenation, and lymphatic drainage.
Improved microcirculatory dynamics favor epidermal turnover and contribute to the progressive normalization of pigment distribution. An essential aspect of this approach is the delivery of active ingredients through trans-epidermal infusion, allowing effective penetration without disruption of the skin barrier or the use of needles. The use of targeted formulations containing high concentrations of vitamin C, such as JetCare Selective Care Lightning and JetCare Med Relight, supports the reduction of oxidative stress, and restoration of cutaneous homeostasis, contributing to improved skin luminosity and pigment stabilization.
In addition, the simultaneous combination of JetPeel and green LED therapy within the 535-545 nm wavelength in the same procedure may further support hyperpigmentation management and improve skin tone uniformity. Integrated into a non-invasive protocol, this combined approach supports long-term pigment balance and skin equilibrium.
CONCLUSION
Pigmentary alterations arise from disrupted cutaneous homeostasis involving melanocyte activation, altered melanin distribution, reduced epidermal turnover, inflammatory signaling, vascular contribution, and barrier dysfunction. Aging further prolongs pigment retention, increasing the persistence of tone irregularities. Hyperpigmentation therefore reflects cumulative biological imbalance rather than isolated melanin overproduction. Non-invasive aesthetic approaches support pigment normalization by enhancing physiological renewal and minimizing inflammatory stress.
JetPeel by TavTech can be integrated as a non-invasive modality that improves microcirculation, epidermal turnover, and the trans-epidermal delivery of targeted active ingredients from JetCare by TavTech such as antioxidants and lightening agents, while preserving skin integrity. By supporting physiological skin functions and maintaining cutaneous equilibrium, this approach aligns biological regulation with aesthetic outcomes and reinforces homeostasis as the central determinant of long-term skin tone uniformity and skin quality.